Begin by carefully reviewing the patient’s medical history, focusing on existing conditions like anxiety disorders, depression, or substance abuse. This foundational step allows for informed decision-making regarding Buspar’s suitability and potential interactions with other medications.
Dosage typically starts low–generally 5 mg twice daily–and is gradually increased based on individual response and tolerability. Close monitoring is crucial during titration, observing for side effects such as dizziness, nausea, or headache. Adjustments are made incrementally, usually over several weeks, to find the optimal therapeutic dose.
Remember that Buspar’s onset of action is gradual, often requiring several weeks to achieve full therapeutic effects. Patient education about this delayed response is key to managing expectations and ensuring adherence to the prescribed regimen. Encourage open communication about any concerns or changes in their condition.
Regular follow-up appointments allow for ongoing assessment of treatment efficacy and side effect management. Consider using validated assessment tools to quantify symptom improvement. This data-driven approach facilitates objective evaluation of treatment response and aids in making necessary adjustments to the treatment plan.
Always consult relevant prescribing information and guidelines before initiating Buspar therapy. Be aware of potential drug interactions and contraindications. This ensures patient safety and optimizes treatment outcomes.
- Buspar Prescribing: A Detailed Guide
- Understanding Buspar’s Role in Anxiety Treatment
- Buspar’s Strengths: A Targeted Approach
- Understanding Limitations and Considerations
- Dosage and Administration of Buspar: A Practical Overview
- Potential Interactions and Contraindications of Buspar
- Medication Interactions
- Contraindications
- Important Note:
- Monitoring Patient Response and Addressing Potential Issues
- Managing Side Effects
- Addressing Lack of Response
- Monitoring for Potential Interactions
- Long-Term Management
Buspar Prescribing: A Detailed Guide
Always begin with a thorough patient history, focusing on anxiety symptoms, duration, and severity. Assess for potential drug interactions, especially with MAO inhibitors and CNS depressants.
Start with a low dose of Buspar (e.g., 5 mg twice daily) to minimize side effects. Gradually increase the dosage over several weeks, monitoring the patient’s response closely. Typical effective doses range from 15-60 mg daily, divided into two or three administrations.
Regularly monitor the patient for therapeutic efficacy and adverse effects. Common side effects include dizziness, nausea, headache, and drowsiness. These usually subside with continued treatment or dose adjustment. Serious side effects are rare but require immediate attention.
Consider the patient’s overall health and other medications when adjusting the dose. Liver or kidney impairment may necessitate dosage reduction. Elderly patients might benefit from lower starting doses.
Encourage open communication between the patient and you regarding symptoms and side effects. Patient education on medication adherence and expected outcomes is critical for successful treatment.
Tapering off Buspar is recommended to prevent withdrawal symptoms. A gradual reduction over several weeks, guided by the patient’s response, is usually sufficient.
Regular follow-up appointments allow for monitoring of treatment effectiveness, adjustment of dosage, and addressing any concerns. Document all clinical findings and treatment decisions meticulously.
Recognize that Buspar’s effects may not be immediate. Therapeutic benefit often takes several weeks to manifest. Be patient and maintain clear communication with the patient throughout this process.
Always consult the latest prescribing information for complete details and updates on Buspar. Stay informed of any new research or guidelines related to its use.
Understanding Buspar’s Role in Anxiety Treatment
Buspar, or buspirone, works differently than many other anxiety medications. It primarily affects serotonin receptors in the brain, reducing anxiety without the sedative effects often associated with benzodiazepines. This means you’re less likely to feel drowsy or experience cognitive impairment.
Buspar’s Strengths: A Targeted Approach
Its unique mechanism makes Buspar a good choice for individuals seeking long-term anxiety management. Unlike benzodiazepines, Buspar doesn’t carry the same risk of dependence or withdrawal symptoms. This is a significant advantage for sustained treatment. Doctors often prescribe it for generalized anxiety disorder (GAD), and it may help manage some symptoms of social anxiety disorder.
Understanding Limitations and Considerations
Buspar takes several weeks to reach full effectiveness. You won’t experience immediate relief like you might with other medications. Also, it may not be as effective for panic attacks or acute anxiety situations. It’s important to discuss your specific needs and expectations with your doctor to ensure Buspar is the right fit for your anxiety treatment plan. Your doctor will consider your medical history and potential interactions with other medications before prescribing it. Always follow your doctor’s instructions regarding dosage and duration of treatment.
Dosage and Administration of Buspar: A Practical Overview
Buspar (buspirone) is typically started at a low dose and gradually increased as needed. Your doctor will personalize your dosage based on your individual response and medical history.
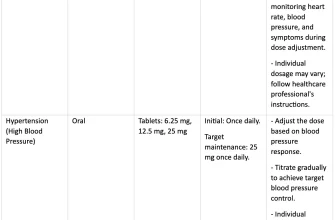
Common starting doses are 5 mg twice daily, or 10 mg once daily. Your physician may increase this by 5 mg every 2-3 days, up to a maximum of 60 mg daily. The full therapeutic effect usually isn’t seen for several weeks.
Buspar is usually taken with food to minimize potential stomach upset. It’s crucial to take it as directed by your doctor. Skipping doses can reduce its efficacy.
| Dosage | Frequency | Notes |
|---|---|---|
| 5 mg | Twice daily | Common starting dose |
| 10 mg | Once daily | Alternative starting dose |
| 15-60 mg | Daily (in divided doses) | Maximum daily dose is 60 mg; divided doses may be used |
Remember, this information is for general knowledge and does not substitute for professional medical advice. Always consult your physician or pharmacist before starting, stopping, or changing your Buspar dosage.
Potential Interactions and Contraindications of Buspar
Always inform your doctor about all medications you take, including over-the-counter drugs, herbal supplements, and recreational drugs. Buspar can interact with several substances, potentially altering its effectiveness or causing adverse effects.
Medication Interactions
- MAO Inhibitors: Avoid combining Buspar with MAO inhibitors (like phenelzine or tranylcypromine). A dangerous reaction can occur. Allow a sufficient drug-free period between stopping an MAOI and starting Buspar, as recommended by your physician.
- Alcohol: Alcohol can enhance Buspar’s sedative effects, leading to increased drowsiness and impaired coordination. Limit or avoid alcohol consumption while taking Buspar.
- CNS Depressants: Combining Buspar with other central nervous system depressants, such as opioids, benzodiazepines, or barbiturates, can increase the risk of sedation, respiratory depression, and other serious complications. Your doctor needs to know about any such medications.
- Grapefruit Juice: Grapefruit juice can interact with Buspar’s metabolism, potentially altering its blood levels. Limit or avoid grapefruit juice consumption while on Buspar.
Contraindications
- Known Allergy: If you have a known allergy to Buspirone or any of its ingredients, you should not take this medication.
- Severe Liver Disease: Buspar is primarily metabolized by the liver. Individuals with severe liver impairment might experience increased side effects. Your doctor will assess your liver function before prescribing Buspar.
- Breastfeeding: Buspar can pass into breast milk. Consult your doctor about breastfeeding while taking this medication, weighing potential risks against benefits.
Important Note:
This information is not exhaustive. Always consult your physician or pharmacist for personalized advice regarding potential interactions and contraindications based on your individual health status and medication regimen. They can provide the most accurate and up-to-date information.
Monitoring Patient Response and Addressing Potential Issues
Schedule regular follow-up appointments to assess treatment progress. Monitor for symptom improvement, noting both the frequency and severity of anxiety symptoms. Track medication adherence, addressing any challenges promptly.
Managing Side Effects
Patients should report any side effects, including dizziness, nausea, headache, or fatigue. Dosage adjustments may alleviate mild side effects. Severe side effects require immediate medical attention. Discuss alternative treatments if side effects are intolerable.
Addressing Lack of Response
If anxiety symptoms don’t improve after four to six weeks of treatment at the prescribed dose, consider increasing the dosage under medical supervision. Alternatively, explore other treatment options, such as adding a different medication or considering therapy. Regularly reassess the treatment plan based on the patient’s response.
Monitoring for Potential Interactions
Inform patients about potential drug interactions with Buspar and other medications, including antidepressants, MAO inhibitors, and certain herbal remedies. Patients should disclose all medications and supplements they are taking. Closely monitor patients for any unusual symptoms or changes in condition.
Long-Term Management
Long-term use of Buspar generally requires ongoing monitoring. Regular check-ups are necessary to assess the continued effectiveness of the medication and to address any emerging issues. Gradual tapering is advised when discontinuing Buspar to prevent withdrawal symptoms.