Coumadin (warfarin) doesn’t treat high blood pressure directly. Its primary function is blood thinning, preventing dangerous clots. Therefore, you won’t use it as a standalone hypertension treatment.
However, certain high blood pressure medications can interact with Coumadin, altering its effectiveness and potentially increasing bleeding risk. These interactions frequently involve drugs like NSAIDs (ibuprofen, naproxen), some antibiotics, and certain antifungals. Your doctor must carefully monitor your Coumadin dosage if you’re also taking any of these.
Regular blood tests are crucial while on Coumadin to maintain the correct therapeutic range. This ensures adequate blood thinning to prevent clots without excessive bleeding. These tests, along with your doctor’s careful monitoring of your blood pressure and medication regimen, are paramount to your safety and health.
Always consult your physician or pharmacist before starting, stopping, or changing any medication, particularly if you’re already taking Coumadin. They can assess potential drug interactions and adjust your medication plan to minimize risks and maximize benefits. Open communication about all your medications is key.
Note: This information is for educational purposes only and does not constitute medical advice. Always consult a qualified healthcare professional for diagnosis and treatment.
- Coumadin for High Blood Pressure: A Comprehensive Overview
- Why the Confusion?
- Potential Interactions:
- Managing Concurrent Medications:
- Important Note:
- Seeking Professional Advice:
- Understanding Coumadin’s Role (or Lack Thereof) in Blood Pressure Management
- Why the Confusion?
- What to Do If You Have Both High Blood Pressure and Are on Coumadin
- High Blood Pressure: Common Causes and Treatment Options
- Lifestyle Changes
- Medication
- Other Factors
- Why Coumadin Isn’t a Blood Pressure Medication
- How Coumadin Works
- Blood Pressure Medications: A Different Approach
- Comparison Table
- Seeking Proper Treatment
- The Relationship Between Blood Clotting and Blood Pressure
- Risk Factors: A Shared Concern
- Managing the Risks
- Potential Interactions Between Coumadin and Blood Pressure Medications
- Increased Bleeding Risk
- Altered Coumadin Effectiveness
- Monitoring and Management
- Individualized Approach
- Managing Blood Pressure and Blood Clotting Simultaneously
- Medication Interactions
- Lifestyle Adjustments
- When to Consult Your Doctor About Coumadin and High Blood Pressure
- Medication Interactions
- Lifestyle Changes and Monitoring
- Signs of Coumadin Overdose or Underdose
- Specific Concerns
- Regular Check-ups
- Important Considerations for Patients on Coumadin
Coumadin for High Blood Pressure: A Comprehensive Overview
Coumadin (warfarin) does not directly treat high blood pressure (hypertension). It’s a blood thinner, preventing blood clots. High blood pressure requires different medications, like ACE inhibitors, beta-blockers, or diuretics.
Why the Confusion?
The misconception arises because some high blood pressure medications, like certain diuretics, can sometimes interact with Coumadin, impacting its effectiveness. This necessitates careful monitoring of your INR (international normalized ratio) – a blood test tracking Coumadin’s impact on clotting.
Potential Interactions:
- Diuretics: Some diuretics, especially thiazide diuretics, can reduce potassium levels, increasing Coumadin’s effects and risk of bleeding. Your doctor will monitor your potassium levels.
- ACE Inhibitors & ARBs: While less common, these drugs can, in some cases, also increase the risk of bleeding when taken with Coumadin. Regular blood tests are key.
Managing Concurrent Medications:
- Open Communication: Inform all your healthcare providers about every medication you take, including over-the-counter drugs and supplements.
- Regular Monitoring: Consistent INR testing is essential to adjust your Coumadin dosage as needed, especially when taking other medications that affect blood clotting or potassium levels.
- Dietary Consistency: Maintain a stable diet. Significant changes in vitamin K intake (found in leafy greens) can influence Coumadin’s effectiveness.
Important Note:
Never adjust your Coumadin dosage without consulting your doctor. Improper dosage can lead to serious complications. Always follow your doctor’s instructions regarding medication and blood tests.
Seeking Professional Advice:
This information is for educational purposes only and shouldn’t replace professional medical advice. Consult your doctor or pharmacist for personalized guidance on managing your high blood pressure and Coumadin therapy.
Understanding Coumadin’s Role (or Lack Thereof) in Blood Pressure Management
Coumadin, or warfarin, doesn’t directly lower blood pressure. Its primary function is blood thinning, preventing blood clots. Therefore, doctors don’t prescribe it to treat hypertension.
Why the Confusion?
Some patients might associate Coumadin with blood pressure management due to overlapping conditions or side effects. For instance, atrial fibrillation, a heart rhythm disorder often treated with Coumadin, can sometimes contribute to high blood pressure. Similarly, certain medications used to manage hypertension may slightly increase the risk of bleeding, a known side effect of Coumadin. This necessitates careful monitoring of both conditions and medications.
What to Do If You Have Both High Blood Pressure and Are on Coumadin
If you’re taking Coumadin and have high blood pressure, your physician will likely prescribe separate medications to address each condition. Discuss your concerns and medication regimen openly with your doctor. They will carefully monitor your blood pressure and INR (international normalized ratio, a measure of your blood’s clotting ability) levels to ensure both your blood pressure and clotting factors remain within the safe range. Regular check-ups are important for coordinating treatments and managing potential interactions.
High Blood Pressure: Common Causes and Treatment Options
High blood pressure, or hypertension, stems from several factors. A major contributor is a diet high in sodium and saturated fats. Regular consumption of processed foods and sugary drinks significantly increases your risk. Lack of physical activity also plays a crucial role; aim for at least 150 minutes of moderate-intensity exercise per week.
Lifestyle Changes
Making dietary changes is key. Reduce sodium intake to less than 2,300 milligrams per day. Choose lean proteins, fruits, vegetables, and whole grains. Weight management is also vital; even a modest weight loss can significantly lower blood pressure. Stress reduction techniques like yoga or meditation can be highly beneficial.
Medication
If lifestyle modifications are insufficient, your doctor might prescribe medication. Common choices include diuretics, which help your body eliminate excess sodium and water, and ACE inhibitors, which relax blood vessels. Beta-blockers and calcium channel blockers are also frequently used. Your doctor will determine the best medication and dosage based on your individual health profile and blood pressure readings. Regular monitoring is important to adjust treatment as needed.
Other Factors
Genetic predisposition increases your chances of developing hypertension. Certain medical conditions, such as kidney disease and sleep apnea, can also contribute. Regular check-ups are essential to detect and manage these underlying issues effectively.
Why Coumadin Isn’t a Blood Pressure Medication
Coumadin (warfarin) thins your blood, preventing clots. It doesn’t directly lower blood pressure. High blood pressure requires different medications.
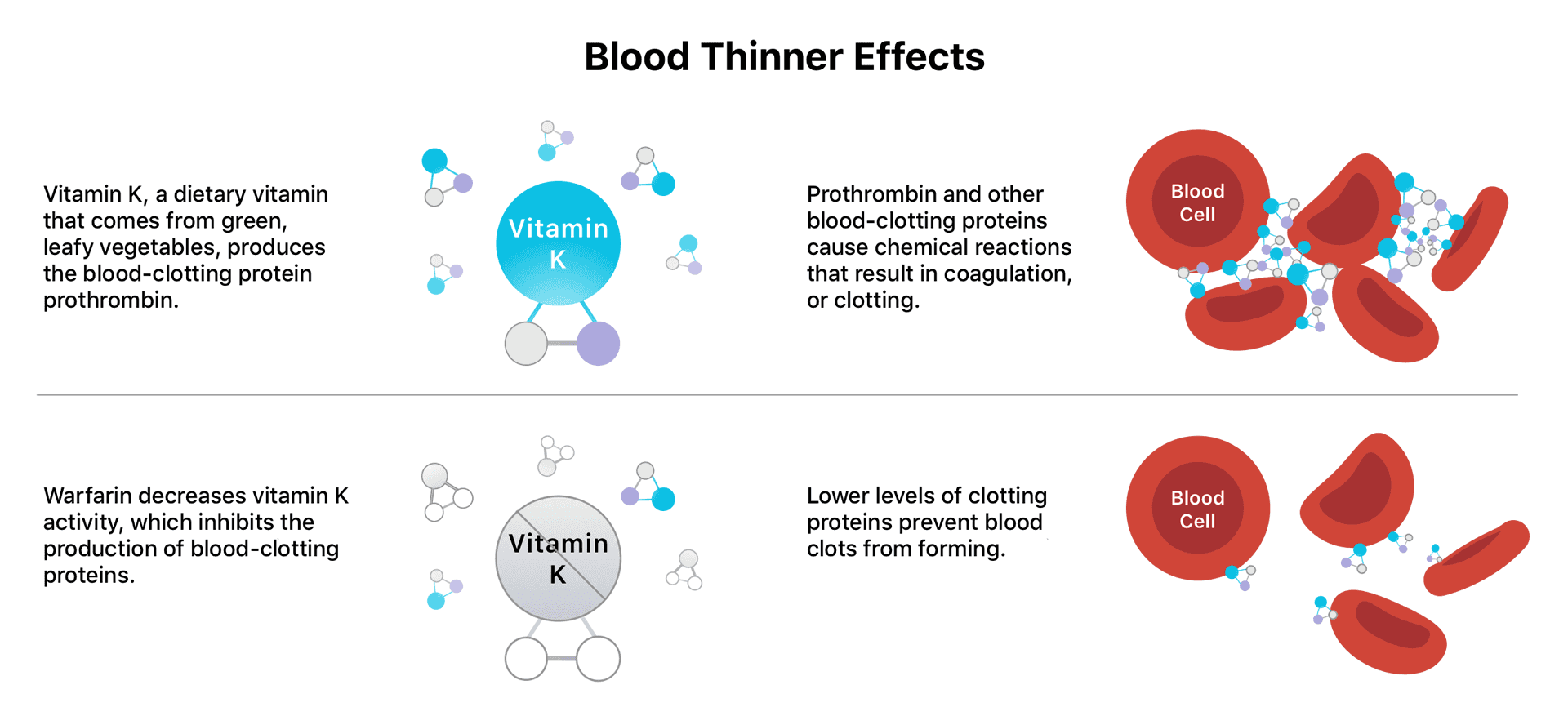
How Coumadin Works
Coumadin works by interfering with vitamin K, a vital factor in blood clotting. This reduces the blood’s ability to form clots, lowering the risk of stroke or heart attack in patients with certain conditions, like atrial fibrillation. It has no impact on the force of your heart’s contractions or the constriction of blood vessels, both key factors in blood pressure regulation.
Blood Pressure Medications: A Different Approach
Blood pressure medications, such as ACE inhibitors, beta-blockers, and diuretics, target the mechanisms that control blood pressure. They either relax blood vessels, decrease heart rate, or reduce blood volume, thus lowering the pressure against your artery walls. These are distinct from Coumadin’s anticoagulant action.
Comparison Table
| Medication Type | Mechanism of Action | Primary Use |
|---|---|---|
| Coumadin (Warfarin) | Inhibits Vitamin K, reducing blood clotting | Stroke prevention in atrial fibrillation, DVT/PE prevention |
| ACE Inhibitors (e.g., Lisinopril) | Relax blood vessels | High blood pressure, heart failure |
| Beta-Blockers (e.g., Metoprolol) | Slow heart rate | High blood pressure, angina |
| Diuretics (e.g., Hydrochlorothiazide) | Reduce blood volume | High blood pressure, fluid retention |
Seeking Proper Treatment
If you have high blood pressure, consult your doctor. They will determine the appropriate medication based on your individual needs and medical history. Never adjust your medication dosage without consulting a healthcare professional. Self-treating can be harmful.
The Relationship Between Blood Clotting and Blood Pressure
High blood pressure doesn’t directly cause blood clots, but they share interconnected risk factors. Think of it like this: high blood pressure damages blood vessel walls. Damaged walls are more prone to clot formation. This damage promotes inflammation, attracting platelets and initiating the clotting cascade. Therefore, managing high blood pressure is vital for cardiovascular health, reducing the risk of both strokes and heart attacks – conditions often linked to blood clots.
Risk Factors: A Shared Concern
Factors like smoking, obesity, diabetes, and high cholesterol increase the risk of both high blood pressure and blood clot formation. These conditions damage blood vessel linings, leading to inflammation and increased clotting risk. For instance, high cholesterol contributes to plaque buildup within arteries, further narrowing them and increasing pressure. This pressure, along with the compromised vessel integrity, increases the likelihood of clot formation. Diabetes, by causing damage to blood vessel walls, similarly enhances the risk. Therefore, addressing these underlying risk factors is key to reducing the probability of complications from both high blood pressure and clotting issues.
Managing the Risks
Regular exercise, a balanced diet rich in fruits and vegetables, and maintaining a healthy weight significantly reduce high blood pressure and the associated clotting risk. Regular monitoring of blood pressure and cholesterol levels is important. Following your doctor’s recommendations for medication, including Coumadin if prescribed, and lifestyle changes are steps towards a healthier cardiovascular system and a reduced risk of blood clots.
Potential Interactions Between Coumadin and Blood Pressure Medications
Taking Coumadin (warfarin) alongside certain blood pressure medications can significantly alter how your body processes either drug, potentially leading to complications. Always inform your doctor about all medications you’re taking, including over-the-counter drugs and supplements.
Increased Bleeding Risk
Several blood pressure medications can increase your risk of bleeding while on Coumadin. This is because some lower blood pressure by affecting blood clotting mechanisms. Increased bleeding risk is a serious concern, and careful monitoring is required.
- NSAIDs (Nonsteroidal Anti-inflammatory Drugs): Ibuprofen and naproxen can increase bleeding risk when combined with Coumadin. Consult your doctor before using these.
- Aspirin: Even low-dose aspirin interacts with Coumadin, increasing bleeding risk. Your doctor will help manage this interaction.
- ACE Inhibitors and ARBs: While less common, some individuals taking these blood pressure medications alongside Coumadin may experience increased bleeding. Regular blood tests are critical for monitoring.
Altered Coumadin Effectiveness
Conversely, some blood pressure medications can affect how well Coumadin works. This can lead to either insufficient blood thinning or an elevated risk of clots.
- Amiodarone: This antiarrhythmic medication can significantly increase Coumadin’s effects, potentially increasing your risk of bleeding. Close monitoring is necessary.
- Rifampin: This antibiotic can decrease Coumadin’s effectiveness, requiring dose adjustments.
- Some diuretics (water pills): Certain diuretics can alter the body’s potassium levels, which in turn can influence how Coumadin works. Your doctor should monitor this interaction closely.
Monitoring and Management
Regular blood tests (INR monitoring) are crucial when taking Coumadin, especially when also taking blood pressure medications. This monitoring helps ensure your Coumadin dosage is appropriate and minimizes risks. Open communication with your physician is key to safely managing these interactions.
Individualized Approach
The interactions between Coumadin and blood pressure medications are highly individual. Factors like age, liver and kidney function, and other health conditions influence the degree of interaction. Your doctor will consider your specific situation to create a safe and effective treatment plan.
Managing Blood Pressure and Blood Clotting Simultaneously
Controlling both high blood pressure and blood clotting requires careful monitoring and a proactive approach. Regular blood tests are critical to track your INR (International Normalized Ratio), measuring how well Coumadin thins your blood. Maintaining a consistent INR within your prescribed range is paramount. Dietary changes play a significant role; consume a balanced diet rich in leafy greens for vitamin K, but avoid sudden, drastic changes. Consistent vitamin K intake helps predict the Coumadin’s effect. Your doctor will provide specific guidance on your dietary needs.
Medication Interactions
Certain medications can interact with Coumadin, affecting its efficacy and potentially raising your blood pressure or increasing bleeding risks. Always inform your doctor and pharmacist about all medications, supplements, and herbal remedies you take. This includes over-the-counter drugs. They can assess potential interactions and adjust your treatment plan accordingly. Regular communication is key.
Lifestyle Adjustments
Lifestyle adjustments can significantly benefit both conditions. Regular exercise, ideally 30 minutes most days of the week, helps lower blood pressure. Stress management techniques, such as yoga or meditation, can also contribute to lower blood pressure and improved overall well-being. Prioritize sufficient sleep, aiming for 7-8 hours nightly. These changes, combined with prescribed medication and medical monitoring, create a robust approach to managing both high blood pressure and blood clotting.
When to Consult Your Doctor About Coumadin and High Blood Pressure
Schedule an appointment immediately if you experience unexplained bleeding or bruising, severe headache, dizziness, or vision changes while taking Coumadin. These could be signs of serious complications.
Contact your doctor if your blood pressure readings consistently remain high despite medication, or if you notice a significant increase in your blood pressure. Regular monitoring is key to managing both conditions effectively.
Medication Interactions
Always inform your doctor about any new medications, supplements, or herbal remedies you start taking. Many substances can interact with Coumadin, potentially impacting its effectiveness or increasing bleeding risk. This includes over-the-counter drugs.
Lifestyle Changes and Monitoring
Report any significant changes in your diet, alcohol consumption, or physical activity level. These factors can influence Coumadin’s effectiveness and your blood pressure. Consistent INR monitoring, as directed by your physician, is crucial for safe management.
Signs of Coumadin Overdose or Underdose
Be aware of the symptoms of Coumadin overdose (excessive bleeding) and underdose (increased risk of blood clots). Promptly report any unusual symptoms to your doctor for appropriate adjustments to your medication dosage.
Specific Concerns
| Symptom | Action |
|---|---|
| Unexplained weight gain | Contact your doctor; this could indicate fluid retention, a potential side effect of some blood pressure medications. |
| Unusual fatigue or weakness | Report these symptoms; they might signal a problem with either your blood pressure or your anticoagulation therapy. |
| Shortness of breath | Seek immediate medical attention; this could indicate a serious complication. |
Regular Check-ups
Attend all scheduled appointments for blood tests and check-ups. Regular monitoring allows your doctor to make necessary adjustments to your medications and ensure your conditions are well-managed.
Important Considerations for Patients on Coumadin
Regularly monitor your INR. Your doctor will provide you with a target range, and consistent monitoring ensures your blood thins appropriately.
Maintain a consistent diet. Significant changes in vitamin K intake can affect your INR. Avoid drastic shifts in leafy green vegetable consumption.
- Keep a food diary to track your intake.
- Consult your doctor or a registered dietitian for personalized dietary advice.
Be aware of potential drug interactions. Many medications can interact with Coumadin, potentially increasing or decreasing its effectiveness. Always inform your doctor and pharmacist of all medications, supplements, and herbal remedies you are taking.
- Bring a list of your medications to every appointment.
- Never start or stop any medication without consulting your doctor.
Report any unusual bleeding or bruising immediately. These can be signs of an elevated INR and require prompt medical attention.
Attend all scheduled appointments. Regular blood tests and check-ups are critical for managing your Coumadin therapy effectively. Your doctor can adjust your dosage based on your INR results.
Understand the signs and symptoms of bleeding complications. These include nosebleeds, easy bruising, heavy menstrual bleeding, and dark, tarry stools. Knowing these symptoms empowers you to act quickly if needed.
Carry a medical alert bracelet or card. This provides crucial information to medical professionals in case of an emergency.
Learn about alternative anticoagulants. New medications are constantly being developed, and discussing these options with your doctor may be beneficial.