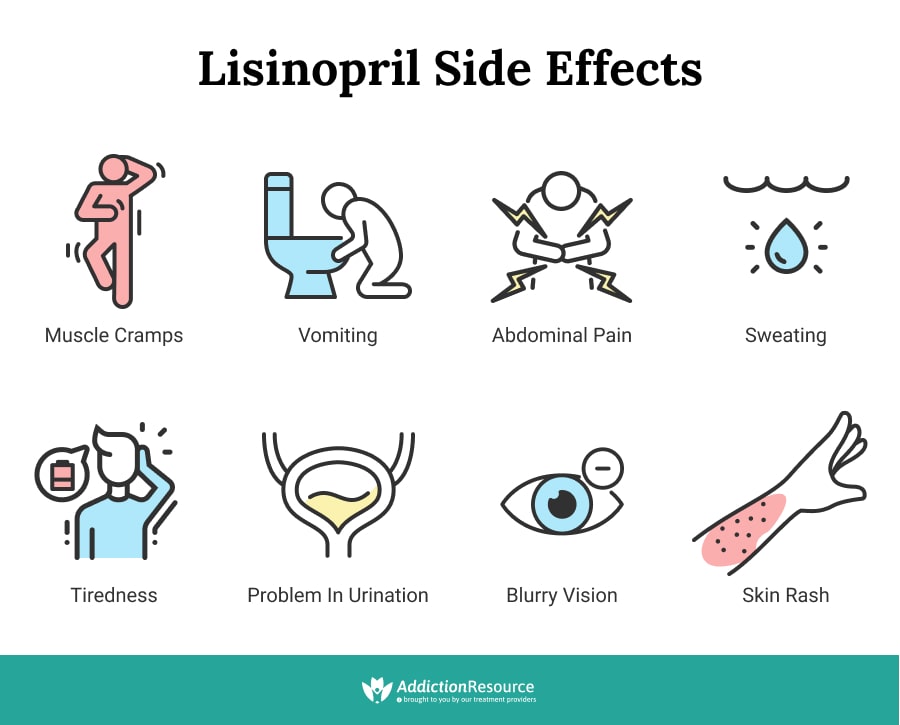
Experiencing low blood pressure while taking Lisinopril? First, understand that this is a common side effect. Many people taking this medication report a drop in blood pressure, particularly during the initial stages of treatment. This usually resolves as your body adjusts, but close monitoring is crucial.
Regularly check your blood pressure at home. Aim for consistent readings to track any significant changes. Keep a record of these readings and share them with your doctor during your follow-up appointments. This allows for timely adjustments to your dosage or medication regimen if needed.
Hydration is key. Dehydration can exacerbate low blood pressure, so make sure you’re drinking plenty of fluids throughout the day. Increasing your salt intake slightly, under your doctor’s guidance, may also help. Do not make these changes independently; consult your physician.
Be aware of symptoms. Dizziness, lightheadedness, fainting, and fatigue are all potential indicators of low blood pressure. If you experience these, contact your doctor immediately. Early intervention prevents serious complications.
Your doctor can help determine the optimal dosage and monitor your response to the medication. They can also discuss alternative treatments if necessary. Open communication is vital for managing this side effect successfully and ensuring your overall health.
- Lisinopril and Low Blood Pressure: A Detailed Guide
- Understanding Lisinopril’s Mechanism and Blood Pressure Reduction
- Reduced Vasoconstriction
- Sodium and Water Excretion
- Individual Responses Vary
- Identifying Symptoms of Low Blood Pressure Caused by Lisinopril
- Managing Lisinopril-Induced Hypotension: Lifestyle Changes
- Medication Adjustments and Interactions to Prevent Low Blood Pressure
- Seeking Medical Attention for Lisinopril-Related Hypotension
- Understanding Your Symptoms
- What to Expect During Your Appointment
Lisinopril and Low Blood Pressure: A Detailed Guide
Monitor your blood pressure regularly, especially during the first few weeks of taking Lisinopril. This allows for early detection of any significant drops.
Understand the symptoms of low blood pressure (hypotension): dizziness, lightheadedness, fainting, nausea. Seek immediate medical attention if you experience these.
Start with a low dose of Lisinopril as prescribed by your doctor. Your doctor will gradually increase the dosage as needed, allowing your body to adjust.
Drink plenty of fluids, especially water. Dehydration can worsen low blood pressure.
Change positions slowly. Avoid sudden movements, especially from lying down or sitting to standing. Take your time getting up from bed or a chair.
Eat regular meals to maintain stable blood sugar levels. Avoid skipping meals, which can lead to blood pressure fluctuations.
Inform your doctor about all medications you are taking, including over-the-counter drugs and supplements, as interactions can affect blood pressure.
Communicate openly with your doctor about any concerns or side effects you experience. They can adjust your medication or treatment plan accordingly.
Consider wearing compression stockings to help improve blood circulation and reduce the risk of low blood pressure, especially if you stand for long periods.
Regular exercise, as recommended by your doctor, can contribute to overall cardiovascular health and help manage blood pressure.
Avoid alcohol consumption, especially excessive amounts, as it can lower blood pressure significantly.
Maintain a healthy diet low in sodium. Sodium intake contributes to high blood pressure, but reducing it too drastically can have unforeseen effects, so discuss this with your doctor.
Understanding Lisinopril’s Mechanism and Blood Pressure Reduction
Lisinopril lowers blood pressure by inhibiting the angiotensin-converting enzyme (ACE). ACE converts angiotensin I to angiotensin II, a potent vasoconstrictor. By blocking ACE, lisinopril reduces angiotensin II levels, causing blood vessels to relax and widen.
Reduced Vasoconstriction
This vasodilation lowers peripheral resistance, reducing the force your heart needs to pump blood. Consequently, blood pressure decreases. This effect is particularly noticeable in patients with high blood pressure.
Sodium and Water Excretion
Lisinopril also increases sodium and water excretion by the kidneys. This reduces blood volume, further contributing to lower blood pressure. The combined effects of vasodilation and reduced blood volume effectively manage hypertension.
Individual Responses Vary
Remember, individual responses to lisinopril vary. Factors like age, overall health, and other medications can influence its effectiveness. Close monitoring by your doctor is crucial for optimal results and safe management of your blood pressure.
Identifying Symptoms of Low Blood Pressure Caused by Lisinopril
Lisinopril lowers blood pressure, sometimes causing it to drop too low. Recognize these symptoms to act quickly:
| Symptom | Description | Action |
|---|---|---|
| Dizziness or Lightheadedness | Feeling faint or unsteady, especially when standing up. | Sit or lie down immediately. |
| Fatigue | Unusual tiredness or weakness. | Rest and avoid strenuous activity. |
| Nausea | Feeling sick to your stomach. | Avoid large meals; sip clear fluids. |
| Blurred Vision | Difficulty focusing or seeing clearly. | Avoid driving or operating machinery. |
| Fainting (Syncope) | Brief loss of consciousness. | Seek medical attention immediately. |
| Headache | Persistent or severe headache. | Rest and hydrate. Consider over-the-counter pain relief (after consulting your doctor). |
| Rapid Pulse | Heart beats faster than normal. | Rest and monitor your heart rate. |
| Confusion | Difficulty thinking clearly or concentrating. | Seek medical advice. |
| Cold, Clammy Skin | Skin feels cool and moist. | Keep warm and stay hydrated. |
If you experience any of these symptoms, contact your doctor immediately. They can adjust your dosage or suggest alternative treatments. Prompt attention can prevent serious complications.
Managing Lisinopril-Induced Hypotension: Lifestyle Changes
Adjust your fluid intake. Dehydration exacerbates low blood pressure. Drink plenty of water throughout the day, aiming for at least eight glasses. Avoid excessive caffeine and alcohol, as these can dehydrate you.
Modify your diet. Increase your sodium intake gradually, under your doctor’s guidance. Small, frequent meals are preferable to three large ones. Focus on foods rich in potassium, like bananas and sweet potatoes, to help regulate blood pressure.
Increase your physical activity slowly. While exercise is beneficial, avoid strenuous activities initially. Start with gentle walks and gradually increase the intensity and duration as tolerated. Listen to your body and rest when needed.
Change positions slowly. Avoid sudden movements, particularly when standing up from a sitting or lying position. Take your time and allow your body to adjust. This reduces the risk of dizziness or fainting.
Monitor your blood pressure regularly. Keep a record of your readings and discuss any significant changes with your doctor. This helps in tracking your progress and making adjustments to your medication or lifestyle as needed. A home blood pressure monitor can be very useful.
Wear compression stockings. These can help improve blood circulation in your legs and reduce the risk of fainting. Consult your doctor before using them.
Maintain a healthy weight. Obesity can contribute to low blood pressure. Losing weight, if necessary, can positively impact blood pressure levels. Talk to your doctor about healthy weight management strategies.
Important Note: These are general recommendations. Always consult your doctor before making any significant changes to your diet, exercise routine, or medication.
Medication Adjustments and Interactions to Prevent Low Blood Pressure
Begin by discussing your concerns with your doctor. They can adjust your Lisinopril dosage gradually to minimize the risk of low blood pressure. A lower starting dose may be appropriate, especially if you have pre-existing conditions.
Careful monitoring of your blood pressure is key. Regular check-ups allow your doctor to make timely adjustments to your medication.
- Keep a blood pressure log to track readings and share with your doctor.
- Report any dizziness, lightheadedness, or fainting immediately.
Certain medications can interact with Lisinopril and increase the risk of low blood pressure. Always inform your doctor and pharmacist about all medications, supplements, and herbal remedies you are taking. This includes over-the-counter drugs like ibuprofen.
- NSAIDs (nonsteroidal anti-inflammatory drugs) can interfere with Lisinopril’s effects.
- Diuretics (water pills) may increase the risk of hypotension when combined with Lisinopril.
- Some antidepressants and antipsychotics can also contribute to low blood pressure when taken with Lisinopril.
Lifestyle changes can help manage blood pressure. These include:
- Regular exercise.
- A balanced diet low in sodium.
- Maintaining a healthy weight.
- Limiting alcohol consumption.
- Quitting smoking.
If you experience low blood pressure, change positions slowly to avoid sudden drops. Sit or lie down until the symptoms subside. Drinking fluids can also help raise blood pressure gradually.
Remember, close communication with your healthcare provider is critical for safe and effective management of your blood pressure while taking Lisinopril.
Seeking Medical Attention for Lisinopril-Related Hypotension
If you experience dizziness, lightheadedness, or fainting after taking Lisinopril, contact your doctor immediately. These are common signs of low blood pressure (hypotension). Don’t hesitate; prompt action is key.
Understanding Your Symptoms
Describe your symptoms clearly to your doctor, including when they occur, their intensity, and any other related symptoms like nausea or blurred vision. Accurate symptom reporting helps your doctor determine the best course of action.
Note the time you took your Lisinopril and when symptoms started. This timeline assists your physician in evaluating the medication’s effect. Keep a record of your blood pressure readings if you have a home monitor. This provides valuable data.
What to Expect During Your Appointment
Your doctor will likely check your blood pressure and heart rate. They may order blood tests to rule out other conditions. Adjusting your Lisinopril dosage or switching medications might be necessary. Discuss any other medications you’re taking, including over-the-counter drugs and supplements, as interactions can influence blood pressure.
Follow your doctor’s instructions carefully. They will provide personalized advice to manage your blood pressure and minimize side effects. Regular follow-up appointments are vital to monitor your progress and make adjustments as needed.